Which Art of the Skin Is the Laer of Areolar Connective Tissue
Learning Objectives
- Identify the components of the integumentary system
- Describe the layers of the skin and the functions of each layer
- Identify and describe the hypodermis and deep fascia
- Describe the role of keratinocytes and their life cycle
- Describe the role of melanocytes in skin pigmentation
Although you may non typically recollect of the skin as an organ, it is in fact fabricated of tissues that work together equally a single structure to perform unique and critical functions. The skin and its accompaniment structures make upwardly theintegumentary system, which provides the body with overall protection. The skin is made of multiple layers of cells and tissues, which are held to underlying structures by connective tissue (Figure one). The deeper layer of skin is well vascularized (has numerous blood vessels). Information technology also has numerous sensory, and autonomic and sympathetic nervus fibers ensuring communication to and from the brain.
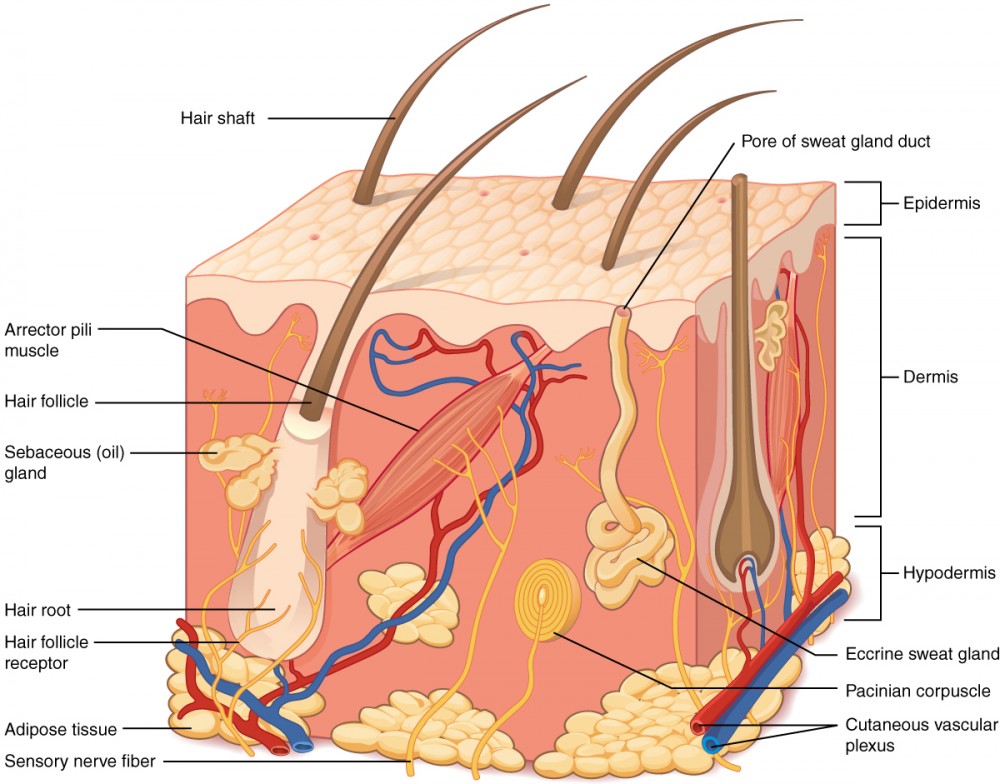
Figure 1. Layers of Pare. The skin is equanimous of 2 chief layers: the epidermis, made of closely packed epithelial cells, and the dermis, made of dense, irregular connective tissue that houses claret vessels, hair follicles, sweat glands, and other structures. Beneath the dermis lies the hypodermis, which is composed mainly of loose connective and fatty tissues.
The peel consists of two main layers and a closely associated layer. View this animation to acquire more nearly layers of the peel. What are the bones functions of each of these layers?
The Epidermis
Theepidermis is composed of keratinized, stratified squamous epithelium. Information technology is made of 4 or 5 layers of epithelial cells, depending on its location in the body. Information technology does not take whatsoever claret vessels within it (i.east., information technology is avascular). Skin that has iv layers of cells is referred to equally "thin pare." From deep to superficial, these layers are the stratum basale, stratum spinosum, stratum granulosum, and stratum corneum. About of the peel can be classified equally thin skin. "Thick skin" is found only on the palms of the easily and the soles of the anxiety. It has a 5th layer, chosen the stratum lucidum, located betwixt the stratum corneum and the stratum granulosum (Figure 2).

Effigy 2. Thin Skin versus Thick Skin. These slides prove cross-sections of the epidermis and dermis of (a) thin and (b) thick skin. Note the pregnant difference in the thickness of the epithelial layer of the thick peel. From height, LM × 40, LM × 40. (Micrographs provided by the Regents of Academy of Michigan Medical School © 2012)
The cells in all of the layers except the stratum basale are chosen keratinocytes. Akeratinocyte is a prison cell that articles and stores the protein keratin.Keratin is an intracellular fibrous poly peptide that gives hair, nails, and skin their hardness and h2o-resistant backdrop. The keratinocytes in the stratum corneum are dead and regularly slough abroad, beingness replaced by cells from the deeper layers (Effigy three).

Figure iii. Epidermis. The epidermis is epithelium composed of multiple layers of cells. The basal layer consists of cuboidal cells, whereas the outer layers are squamous, keratinized cells, so the whole epithelium is ofttimes described as beingness keratinized stratified squamous epithelium. LM × 40. (Micrograph provided by the Regents of University of Michigan Medical School © 2012)
View the University of Michigan WebScope at to explore the tissue sample in greater detail. If y'all zoom on the cells at the outermost layer of this department of pare, what do y'all detect nearly the cells?
Stratum Basale
Thestratum basale (also called the stratum germinativum) is the deepest epidermal layer and attaches the epidermis to the basal lamina, beneath which prevarication the layers of the dermis. The cells in the stratum basale bond to the dermis via intertwining collagen fibers, referred to as the basement membrane. A finger-similar projection, or fold, known equally the dermal papilla (plural = dermal papillae) is constitute in the superficial portion of the dermis. Dermal papillae increase the force of the connection between the epidermis and dermis; the greater the folding, the stronger the connections made (Figure iv).
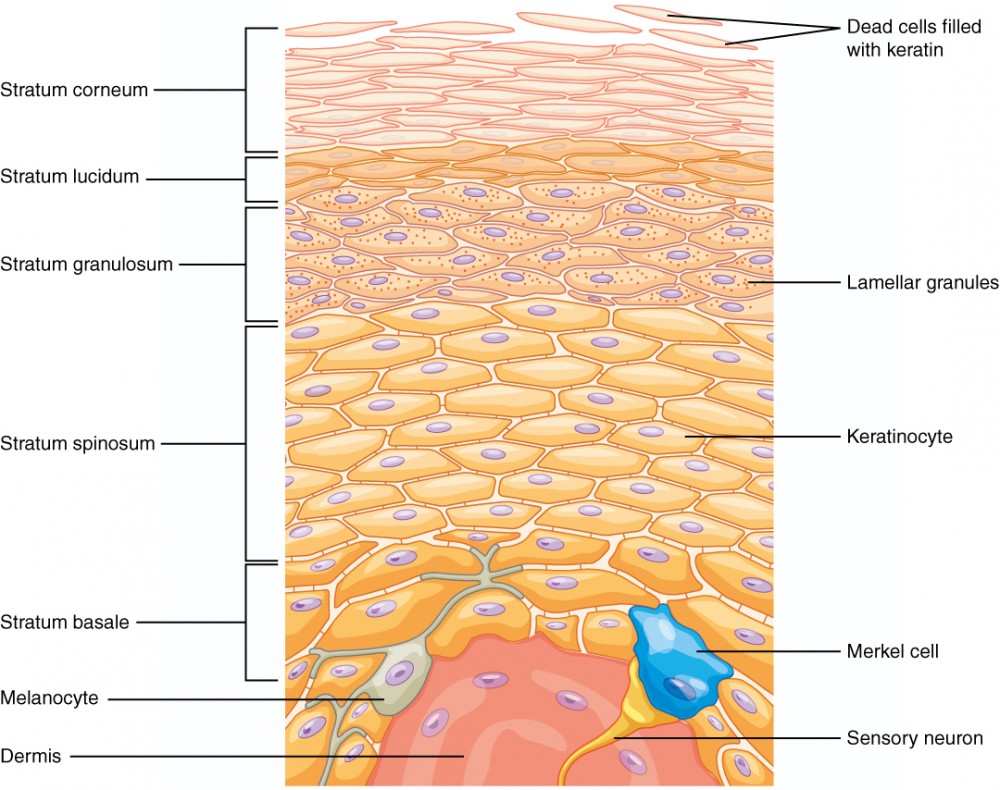
Figure four. Layers of the Epidermis. The epidermis of thick pare has five layers: stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum.
The stratum basale is a single layer of cells primarily made of basal cells. Abasal cell is a cuboidal-shaped stem cell that is a precursor of the keratinocytes of the epidermis. All of the keratinocytes are produced from this unmarried layer of cells, which are constantly going through mitosis to produce new cells. Every bit new cells are formed, the existing cells are pushed superficially away from the stratum basale. Two other cell types are found dispersed amongst the basal cells in the stratum basale. The start is aMerkel cell, which functions as a receptor and is responsible for stimulating sensory nerves that the encephalon perceives as touch. These cells are especially abundant on the surfaces of the hands and feet. The 2d is a melanocyte, a cell that produces the paint melanin.Melanin gives hair and skin its color, and also helps protect the living cells of the epidermis from ultraviolet (UV) radiations damage.
In a growing fetus, fingerprints form where the cells of the stratum basale run into the papillae of the underlying dermal layer (papillary layer), resulting in the germination of the ridges on your fingers that you recognize every bit fingerprints. Fingerprints are unique to each individual and are used for forensic analyses because the patterns practise not alter with the growth and aging processes.
Stratum Spinosum
As the name suggests, thestratum spinosum is spiny in appearance due to the protruding cell processes that join the cells via a construction called adesmosome. The desmosomes interlock with each other and strengthen the bond between the cells. It is interesting to note that the "spiny" nature of this layer is an artifact of the staining process. Unstained epidermis samples do not showroom this feature appearance. The stratum spinosum is composed of eight to 10 layers of keratinocytes, formed as a result of cell division in the stratum basale (Figure 5). Interspersed amongst the keratinocytes of this layer is a type of dendritic cell called theLangerhans cell, which functions every bit a macrophage by engulfing bacteria, foreign particles, and damaged cells that occur in this layer.

Figure 5. Cells of the Epidermis. The cells in the dissimilar layers of the epidermis originate from basal cells located in the stratum basale, yet the cells of each layer are distinctively unlike. EM × 2700. (Micrograph provided by the Regents of Academy of Michigan Medical Schoolhouse © 2012)
View the University of Michigan WebScope to explore the tissue sample in greater detail. If you lot zoom on the cells at the outermost layer of this department of skin, what do yous notice about the cells?
The keratinocytes in the stratum spinosum begin the synthesis of keratin and release a h2o-repelling glycolipid that helps prevent water loss from the body, making the skin relatively waterproof. Every bit new keratinocytes are produced atop the stratum basale, the keratinocytes of the stratum spinosum are pushed into the stratum granulosum.
Stratum Granulosum
Thestratum granulosum has a grainy appearance due to further changes to the keratinocytes as they are pushed from the stratum spinosum. The cells (3 to 5 layers deep) go flatter, their cell membranes thicken, and they generate big amounts of the proteins keratin, which is fibrous, andkeratohyalin, which accumulates as lamellar granules within the cells (run across Figure four). These two proteins brand up the majority of the keratinocyte mass in the stratum granulosum and give the layer its grainy advent. The nuclei and other cell organelles disintegrate as the cells dice, leaving behind the keratin, keratohyalin, and cell membranes that will class the stratum lucidum, the stratum corneum, and the accessory structures of pilus and nails.
Stratum Lucidum
Thestratum lucidum is a smooth, seemingly translucent layer of the epidermis located just above the stratum granulosum and beneath the stratum corneum. This thin layer of cells is found only in the thick peel of the palms, soles, and digits. The keratinocytes that compose the stratum lucidum are dead and flattened (run into Figure iv). These cells are densely packed witheleiden, a clear protein rich in lipids, derived from keratohyalin, which gives these cells their transparent (i.e., lucid) appearance and provides a barrier to water.
Stratum Corneum
Thestratum corneum is the nigh superficial layer of the epidermis and is the layer exposed to the outside environment (come across Figure 4). The increased keratinization (also chosen cornification) of the cells in this layer gives information technology its name. There are usually 15 to thirty layers of cells in the stratum corneum. This dry, dead layer helps prevent the penetration of microbes and the dehydration of underlying tissues, and provides a mechanical protection confronting abrasion for the more delicate, underlying layers. Cells in this layer are shed periodically and are replaced past cells pushed up from the stratum granulosum (or stratum lucidum in the case of the palms and soles of feet). The entire layer is replaced during a flow of almost iv weeks. Cosmetic procedures, such equally microdermabrasion, help remove some of the dry, upper layer and aim to keep the peel looking "fresh" and good for you.
Dermis
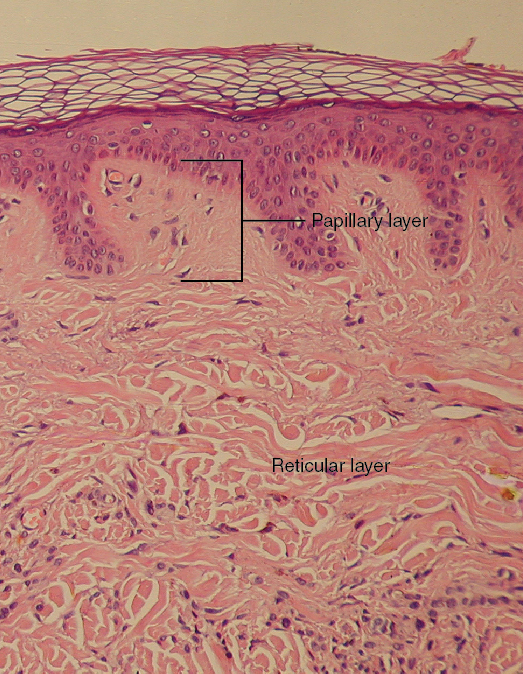
Figure half-dozen. Layers of the Dermis. This stained slide shows the two components of the dermis—the papillary layer and the reticular layer. Both are made of connective tissue with fibers of collagen extending from one to the other, making the border betwixt the 2 somewhat indistinct. The dermal papillae extending into the epidermis belong to the papillary layer, whereas the dense collagen fiber bundles below belong to the reticular layer. LM × 10. (credit: modification of work by "kilbad"/Wikimedia Commons)
Thedermis might be considered the "core" of the integumentary organisation (derma– = "skin"), equally distinct from the epidermis (epi– = "upon" or "over") and hypodermis (hypo– = "below"). It contains blood and lymph vessels, nerves, and other structures, such as hair follicles and sweat glands. The dermis is made of 2 layers of connective tissue that etch an interconnected mesh of elastin and collagenous fibers, produced past fibroblasts (Figure half dozen).
Papillary Layer
Thepapillary layer is made of loose, areolar connective tissue, which means the collagen and elastin fibers of this layer form a loose mesh. This superficial layer of the dermis projects into the stratum basale of the epidermis to form finger-like dermal papillae (come across Effigy six). Within the papillary layer are fibroblasts, a small number of fatty cells (adipocytes), and an affluence of small blood vessels. In add-on, the papillary layer contains phagocytes, defensive cells that assistance fight bacteria or other infections that have breached the peel. This layer also contains lymphatic capillaries, nerve fibers, and touch on receptors called the Meissner corpuscles.
Reticular Layer
Underlying the papillary layer is the much thickerreticular layer, composed of dense, irregular connective tissue. This layer is well vascularized and has a rich sensory and sympathetic nervus supply. The reticular layer appears reticulated (internet-like) due to a tight meshwork of fibers.Elastin fibers provide some elasticity to the skin, enabling move. Collagen fibers provide construction and tensile strength, with strands of collagen extending into both the papillary layer and the hypodermis. In addition, collagen binds water to continue the skin hydrated. Collagen injections and Retin-A creams help restore skin turgor by either introducing collagen externally or stimulating blood menstruum and repair of the dermis, respectively.
Hypodermis
Thehypodermis (likewise chosen the subcutaneous layer or superficial fascia) is a layer directly beneath the dermis and serves to connect the skin to the underlying fascia (fibrous tissue) of the basic and muscles. It is not strictly a office of the pare, although the border between the hypodermis and dermis can be difficult to distinguish. The hypodermis consists of well-vascularized, loose, areolar connective tissue and adipose tissue, which functions every bit a manner of fat storage and provides insulation and cushioning for the integument.
Everyday Connectedness: Lipid Storage
The hypodermis is home to most of the fat that concerns people when they are trying to proceed their weight nether control. Adipose tissue present in the hypodermis consists of fat-storing cells chosen adipocytes. This stored fatty can serve as an free energy reserve, insulate the torso to prevent estrus loss, and human action as a cushion to protect underlying structures from trauma.
Where the fat is deposited and accumulates within the hypodermis depends on hormones (testosterone, estrogen, insulin, glucagon, leptin, and others), every bit well as genetic factors. Fat distribution changes as our bodies mature and age. Men tend to accumulate fat in different areas (neck, arms, lower back, and abdomen) than do women (breasts, hips, thighs, and buttocks). The trunk mass index (BMI) is frequently used as a measure of fat, although this measure is, in fact, derived from a mathematical formula that compares body weight (mass) to acme. Therefore, its accurateness equally a health indicator can be called into question in individuals who are extremely physically fit.
In many animals, there is a blueprint of storing excess calories equally fat to be used in times when food is not readily available. In much of the developed world, insufficient exercise coupled with the ready availability and consumption of high-calorie foods have resulted in unwanted accumulations of adipose tissue in many people. Although periodic aggregating of excess fatty may take provided an evolutionary reward to our ancestors, who experienced unpredictable bouts of famine, information technology is now becoming chronic and considered a major health threat. Recent studies bespeak that a distressing pct of our population is overweight and/or clinically obese. Not only is this a problem for the individuals affected, just it also has a severe impact on our healthcare system. Changes in lifestyle, specifically in diet and exercise, are the all-time ways to control torso fat accumulation, peculiarly when it reaches levels that increase the risk of heart affliction and diabetes.
Pigmentation
The color of peel is influenced by a number of pigments, including melanin, carotene, and hemoglobin. Recall that melanin is produced by cells called melanocytes, which are found scattered throughout the stratum basale of the epidermis. The melanin is transferred into the keratinocytes via a cellular vesicle called amelanosome (Effigy 7).

Figure 7. Skin Pigmentation. The relative coloration of the peel depends of the corporeality of melanin produced by melanocytes in the stratum basale and taken up by keratinocytes.
Melanin occurs in two primary forms. Eumelanin exists every bit black and brownish, whereas pheomelanin provides a red colour. Dark-skinned individuals produce more melanin than those with pale skin. Exposure to the UV rays of the sun or a tanning salon causes melanin to be manufactured and built up in keratinocytes, every bit sun exposure stimulates keratinocytes to secrete chemicals that stimulate melanocytes. The accumulation of melanin in keratinocytes results in the concealment of the skin, or a tan. This increased melanin accumulation protects the Dna of epidermal cells from UV ray impairment and the breakup of folic acrid, a nutrient necessary for our health and well-being. In contrast, too much melanin can interfere with the product of vitamin D, an of import nutrient involved in calcium absorption. Thus, the amount of melanin present in our peel is dependent on a residuum between available sunlight and folic acid destruction, and protection from UV radiations and vitamin D product.
It requires well-nigh 10 days after initial lord's day exposure for melanin synthesis to acme, which is why pale-skinned individuals tend to suffer sunburns of the epidermis initially. Dark-skinned individuals can as well go sunburns, but are more protected than are pale-skinned individuals. Melanosomes are temporary structures that are eventually destroyed by fusion with lysosomes; this fact, along with melanin-filled keratinocytes in the stratum corneum sloughing off, makes tanning impermanent.
Likewise much sun exposure can eventually pb to wrinkling due to the devastation of the cellular structure of the skin, and in severe cases, can cause sufficient DNA impairment to result in skin cancer. When there is an irregular accumulation of melanocytes in the skin, freckles appear. Moles are larger masses of melanocytes, and although most are benign, they should be monitored for changes that might indicate the presence of cancer (Figure 8).

Effigy viii. Moles range from benign accumulations of melanocytes to melanomas. These structures populate the landscape of our skin. (credit: the National Cancer Found)
Key Takeaways
Disorders of the Integumentary System
The offset thing a clinician sees is the pare, and then the examination of the pare should be part of any thorough physical test. Most peel disorders are relatively beneficial, but a few, including melanomas, can be fatal if untreated. A couple of the more noticeable disorders, albinism and vitiligo, impact the advent of the peel and its accessory organs. Although neither is fatal, it would be hard to merits that they are benign, at least to the individuals and then afflicted.

Effigy ix. Vitiligo. Individuals with vitiligo feel depigmentation that results in lighter colored patches of skin. The condition is especially noticeable on darker skin. (credit: Klaus D. Peter)
Albinism is a genetic disorder that affects (completely or partially) the coloring of skin, pilus, and eyes. The defect is primarily due to the inability of melanocytes to produce melanin. Individuals with albinism tend to announced white or very pale due to the lack of melanin in their skin and hair. Recall that melanin helps protect the skin from the harmful effects of UV radiation. Individuals with albinism tend to need more than protection from UV radiations, every bit they are more prone to sunburns and skin cancer. They too tend to be more sensitive to light and accept vision problems due to the lack of pigmentation on the retinal wall. Treatment of this disorder normally involves addressing the symptoms, such as limiting UV light exposure to the skin and eyes. Invitiligo, the melanocytes in sure areas lose their ability to produce melanin, perchance due to an autoimmune reaction. This leads to a loss of colour in patches (Figure 9). Neither albinism nor vitiligo directly affects the lifespan of an individual.
Other changes in the appearance of pare coloration can be indicative of diseases associated with other body systems. Liver disease or liver cancer tin can cause the accumulation of bile and the yellow paint bilirubin, leading to the skin appearing yellowish or jaundiced (jaune is the French word for "xanthous"). Tumors of the pituitary gland can result in the secretion of large amounts of melanocyte-stimulating hormone (MSH), which results in a darkening of the skin. Similarly, Addison'south disease can stimulate the release of excess amounts of adrenocorticotropic hormone (ACTH), which can requite the peel a deep bronze color. A sudden drop in oxygenation tin affect peel color, causing the skin to initially plough ashen (white). With a prolonged reduction in oxygen levels, dark red deoxyhemoglobin becomes ascendant in the claret, making the skin appear blueish, a condition referred to every bit cyanosis (kyanos is the Greek discussion for "blue"). This happens when the oxygen supply is restricted, as when someone is experiencing difficulty in breathing because of asthma or a heart attack. However, in these cases the event on pare color has cipher do with the skin'southward pigmentation.
This ABC video follows the story of a pair of fraternal African-American twins, ane of whom is albino. Watch this video to learn about the challenges these children and their family face up. Which ethnicities practise yous think are exempt from the possibility of albinism?
Cocky-Check Questions
Have the quiz below to bank check your agreement of the Layers of the Skin:
Source: https://courses.lumenlearning.com/suny-ap1/chapter/layers-of-the-skin/
0 Response to "Which Art of the Skin Is the Laer of Areolar Connective Tissue"
Post a Comment